PCOS lean often goes unnoticed because the body looks stable while hormones shift quietly in the background. Small signs appear early, but they rarely look serious enough to explain the deeper changes underway.
Doctors now understand these hidden patterns more clearly and point to the corrections that create steady progress. Their perspective offers a clearer way to approach symptoms that never seemed obvious.
What Lean PCOS Means?
Lean PCOS is a form of polycystic ovarian syndrome that appears in women with a normal weight yet shows the same symptoms seen in typical PCOS. Irregular periods, menstrual irregularities, hair growth changes, and shifts in male hormones and reproductive hormones still occur despite a lean appearance.
Understanding this definition helps clarify how the condition behaves beneath the surface.
How Lean PCOS Works Internally
The condition alters hormone communication between the brain and ovaries. Reproductive hormones lose their monthly rhythm and androgen activity increases, which disrupts ovulation. These internal shifts follow the same logic seen in broader PCOS patterns, only without external weight based cues.
How Lean PCOS Differs From Classic PCOS
Lean PCOS presents the same hormonal imbalance without the typical weight based cues. Symptoms follow the same biological pathway, yet the external picture appears healthy which leads many women to overlook early changes.
The difference lies in visibility rather than physiology, which makes careful observation more important in lean cases.
Symptoms Often Overlooked in Lean PCOS
-
Light but persistent irregular periods that seem easy to explain as stress.
-
Acne along the jawline or chin linked to androgen excess.
-
Mild scalp thinning or increased facial hair caused by male hormones.
-
Subtle cycle changes that appear normal for age but reflect hormonal drift.
Cycle Markers That Reflect Lean PCOS
-
Irregular periods that arrive late, early or with unpredictable flow.
-
Menstrual cycles that shorten, lengthen or skip without a clear cause.
-
Patterns that resemble non obese pcos even when symptoms appear mild.
Androgen Related Signs
-
Increased hair growth on the face, chest or abdomen influenced by male hormones.
-
Acne or scalp thinning linked to androgen excess.
-
Skin texture changes that mirror typical pcos women.
Ovarian and Hormonal Features
-
Ovarian changes consistent with polycystic ovarian syndrome pcos on ultrasound.
-
Reproductive hormones that shift away from normal ovulation timing.
-
Subtle disruptions that match early pcos characteristics in both obese pcos and lean women.
Why Lean PCOS Often Gets Missed
Lean women are not expected to show symptoms of polycystic ovary syndrome, so irregular periods or extra hair growth are often explained away as stress or temporary imbalance. Because the weight looks stable, pcos complications and cycle irregularities continue for years without deeper investigation.
Clinical Example
A woman in her mid twenties may have a normal weight yet notice irregular menstrual cycle changes and acne concentrated around the jawline. Her symptoms are mild enough to be dismissed as normal. Inside her system, the hormonal profile matches lean polycystic ovary syndrome(pcos), but the absence of weight gain masks its presence.
Lean PCOS is a hormonal condition that affects ovulation, androgen activity and menstrual timing, not a weight dependent disorder.
Recognising this distinction builds the right foundation for understanding how lean PCOS connects to insulin patterns and wider metabolic disorders, which is the next step in this picture.
Why Lean PCOS Raises Insulin Resistance And Metabolic Disorders Risk?
Lean women can still face impaired glucose tolerance, elevated serum insulin, insulin resistant patterns, metabolic abnormalities, and a higher risk of cardiovascular disease. These changes often develop quietly, without excess weight or abdominal fat.
Seeing how these metabolic shifts unfold helps explain why symptoms escalate even when body weight appears stable.
How Insulin Resistance Develops In Lean PCOS
In lean PCOS, cells respond less effectively to insulin even when body fat looks normal. Serum insulin and insulin levels rise to keep blood sugar within range, which places constant strain on glucose metabolism.
Over time, this pattern forms the base of insulin resistant profiles that might never be linked to appearance.
Blood Sugar, Glucose Metabolism And Hidden Strain
The body works harder to keep blood sugar stable when insulin resistance begins. This can show up as:
-
Energy dips after meals that feel stronger than expected.
-
Hunger returning quickly even after balanced food choices.
-
Mild shakiness or irritability when meals are delayed.
These signals often appear long before diabetes mellitus or impaired glucose tolerance show on blood tests, yet they already point to pressure on glucose metabolism in lean PCOS women.
From Metabolic Abnormalities To Metabolic Disorders
When metabolic abnormalities persist, the risk of formal metabolic disorders increases. Elevated serum insulin, insulin resistant tendencies and subtle changes in blood sugar regulation can move toward diabetes metab disord patterns if they remain unaddressed.
This shift does not depend on visible excess weight, it depends on how long the system has been under strain.
Role Of Body Fat And Abdominal Fat In Lean Women
Even in lean women, fat distribution matters more than the number on the scale. Small increases in abdominal fat or visceral adipose tissue can worsen insulin resistance and metabolic risk more than overall body weight changes.
Someone may appear slim, yet carry enough central fat to influence cardiovascular disease risk.
Cardiovascular Disease And Long Term Risk
Metabolic disorders linked to lean PCOS increase the chance of high blood pressure, heart disease and broader cardiovascular disease over time. These risks grow quietly when impaired glucose tolerance and insulin resistant patterns go unnoticed.
The combination of hormonal disruption and metabolic strain explains why lean PCOS affects more than periods and skin.
Example: Early Metabolic Changes In A Lean Woman
A woman in her late twenties may maintain a healthy weight yet feel unusually tired after lunch, crave sweets in the afternoon and notice mild blood pressure rises during routine checks. Her lab results still fall near normal, so concerns are set aside.
In reality, her pattern reflects early metabolic abnormalities tied to lean PCOS.
When insulin resistance and metabolic disorders are seen as part of lean PCOS rather than separate issues, testing and follow up become more precise. That clarity is what shapes how doctors approach diagnosis in lean patients and why the evaluation process needs careful attention.
“Take the 2-Minute PCOS Nutrition Assessment”
How Doctors Diagnose PCOS Accurately in Lean Patients?
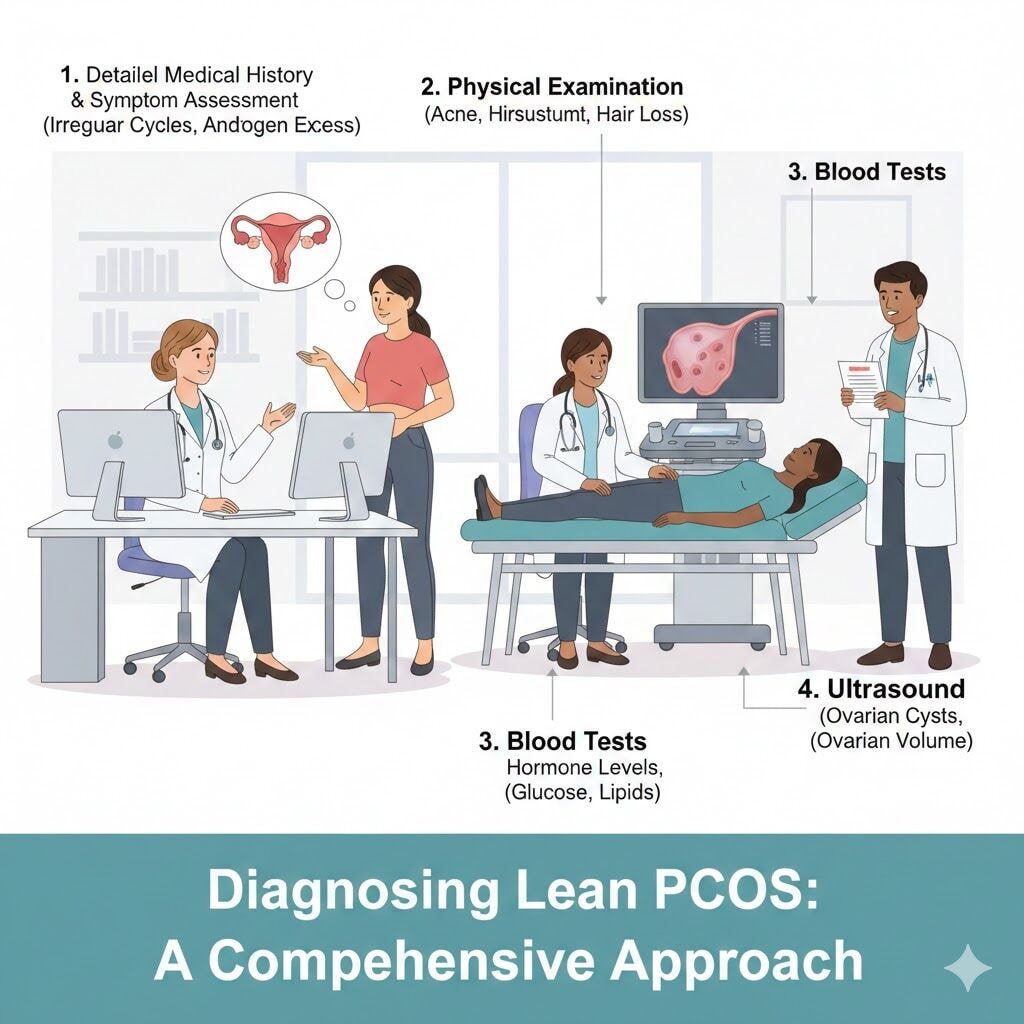
Diagnosis relies on recognising pcos diagnosis criteria beyond body mass index readings and body weight alone. Doctors evaluate healthy bmi ranges, reproductive hormones, androgen excess, and risk factors that point toward polycystic ovarian patterns.
This approach helps avoid misdiagnosis in women who do not show typical outward signs.
What Doctors Look At Beyond Weight
For lean patients, doctors cannot rely on excess weight as a clue. They study patterns across symptoms, lab results and history to diagnose pcos accurately. The focus shifts from appearance to how hormones behave over time in pcos women and lean women with similar complaints.
Core Diagnostic Criteria In Lean PCOS
Most clinicians use adaptations of standard PCOS criteria for lean patients. These typically examine:
-
Evidence of ovulatory dysfunction, such as irregular cycles or infrequent periods.
-
Clinical or lab signs of androgen excess, including acne, hair growth or raised androgen levels.
-
Ovarian changes on ultrasound that suggest a polycystic pattern.
In lean women, these criteria matter more than any change in body weight or body mass index.
Role Of Hormone Tests
Hormone tests help doctors move from suspicion to clarity. They measure reproductive hormones, including those that drive ovulation, and look for imbalance that matches a PCOS profile.
Patterns of androgen excess confirm that symptoms like hair growth or persistent acne come from hormone changes, not only from lifestyle or stress.
Why BMI Alone Is Not Enough
A healthy bmi can give a false sense of reassurance in both pcos patients and clinicians. Many lean patients fall within normal body mass index ranges while still showing strong hormonal signs of PCOS.
For this reason, doctors treat BMI as one piece of context, not a deciding factor when they diagnose pcos.
Identifying Risk Factors In Lean Patients
Doctors also look at risk factors that increase the chance of PCOS in lean patients. These can include a family history of pcos women, menstrual irregularities from early adolescence, or early signs of metabolic strain.
Considering these elements together helps clinicians identify lean polycystic patterns that would otherwise remain hidden.
Ultrasound And Ovarian Features
Imaging supports the diagnosis by showing whether the ovaries follow a polycystic pattern. For some lean patients, ultrasound reveals enlarged ovaries or a higher number of small follicles.
These findings, combined with reproductive hormone results, give a structured view of how closely the picture matches established PCOS characteristics.
Example: How A Lean Woman Receives A Clear Diagnosis
A lean woman in her late twenties arrives with irregular periods, mild jawline acne and new facial hair growth. Her body weight and healthy bmi appear normal, so earlier visits focused on stress and routine changes.
When a specialist reviews her history, orders hormone tests and performs an ultrasound, the combined evidence confirms a PCOS diagnosis in a lean patient.
Once the diagnostic picture is clear, the focus naturally shifts to what lean PCOS women can track on their own, from symptoms to metabolic markers, so that daily choices support the treatment plan instead of working against it.
Steps to Track Symptoms And Metabolic Markers in Lean PCOS Women Effectively
Tracking menstrual cycles, insulin levels, glucose metabolism, body fat trends, and blood pressure gives lean women a practical way to monitor changes early. These markers highlight how symptoms evolve and when intervention becomes necessary.
Keeping consistent logs builds a clearer understanding of the body’s shifting rhythm.
1. Record Menstrual Cycle Patterns Consistently
Tracking cycles helps detect early disruptions such as an irregular menstrual cycle or irregular menstruation often linked to polycystic ovarian syndrome. These subtle shifts reveal how hormones fluctuate across reproductive age and why patterns change over time.
Recording details consistently strengthens awareness of body rhythm and emerging cycle irregularities.
2. Track Daily Energy Levels And Mood Changes
Daily mood and energy shifts often correlate with changes in androgen concentrations and the body’s response to stress. Evaluating these patterns helps identify early hormonal imbalance before broader pcos characteristics appear.
Tracking these subtle differences builds clarity around how emotional and physical responses shape lean PCOS symptoms.
3. Monitor Blood Sugar Responses After Key Meals
Monitoring post meal responses highlights risks associated with diabetes mellitus, diabetes metab disord, and j diabetes metab disord. These patterns show how blood sugar behaves throughout the day and reveal early metabolic strain even in non obese pcos presentations.
Observing these reactions helps refine dietary choices that support stability.
4. Log Signs Of Insulin Resistance Regularly
Noticing early metabolic changes helps prevent complications tied to obese phenotype and obese pcos patterns, even when outward weight changes are absent. Subtle signs often precede visible shifts, revealing how metabolic pressure builds over time.
Tracking these markers helps identify increased risk before symptoms escalate.
5. Note Skin, Hair, And Acne Fluctuations
Shifts in hair growth or breakouts can reflect imbalances influenced by male hormones called androgens. These outward signs often appear in both obese women and overweight women, even when body composition differs.
Observing these patterns provides early clues about hormonal shifts affecting skin and hair.
6. Track Weight, Waist Measurements, And Body Fat Trends
Monitoring body composition helps detect gradual weight gain, abdominal changes linked to adipose tissue, and buildup of visceral adipose tissue that may appear even in lean PCOS cases.
These markers show how metabolic stress develops, especially when moderate weight fluctuations begin influencing hormone function.
7. Monitor Exercise Performance And Recovery
Exercise response can shift unexpectedly for women navigating pcos complications. Even small changes in endurance or recovery highlight how metabolic and hormonal patterns evolve over time.
Observing these variations helps create a clearer picture of how physical activity interacts with internal health markers.
8. Record Sleep Duration And Sleep Quality
Poor sleep can amplify metabolic strain and contribute to conditions seen in obese subjects or individuals with increased risk for systemic imbalance. Observing sleep patterns helps identify early disruptions that may influence hormonal cycles and daily energy levels in lean PCOS.
9. Track Digestive Patterns And Bloating Episodes
Digestive discomfort can accompany metabolic shifts often associated with heart disease risks or broader systemic changes. Tracking digestion helps reveal how food intake affects inflammation or bloating, particularly when underlying metabolic tendencies influence gut responses in lean PCOS.
10. Note Changes In Cravings And Appetite Signals
Craving patterns often reflect deeper hormonal shifts tied to reproductive age and internal metabolic changes. These tendencies may mimic patterns seen in obese pcos patients despite normal outward appearance.
Observing appetite signals helps create clarity around how internal cues guide eating behavior.
Example: Bringing All The Data Together
A lean woman might log two months of cycle dates, post meal energy dips, slight weight gain around the waist and later bedtimes during stressful weeks.
When she reviews these notes with her doctor, the combined pattern reveals early metabolic abnormalities that one isolated symptom could not show on its own.
Once these tracking habits are in place, the next logical step is choosing daily food and movement changes that support insulin sensitivity and safe weight management rather than working against the patterns the body is already revealing.
Tips for Safe Weight Management And Better Insulin Sensitivity For Lean PCOS Women

Effective strategies include focusing on weight loss goals that support glucose metabolism, a healthy diet, targeted dietary interventions, and increasing nutritional intake where needed. These steps help manage pcos symptoms without pushing the body into stress.
1. Prioritize Low Glycemic Index Meals
Choosing meals with steady glucose impact helps reduce long term complications associated with pcos characteristics and impaired hormone balance.
These supportive choices also help lean PCOS women avoid fluctuations seen in moderate weight shifts or broader metabolic patterns. Consistent meal structure strengthens stability throughout the day.
2. Maintain Steady Meal Timings Daily
Regular eating patterns protect against metabolic strain seen in obese phenotype cases, even when outward appearance suggests healthy function.
Balanced timing strengthens digestive rhythm and reduces the likelihood of unpredictable energy drops. Predictable meal spacing supports long term hormone stability.
3. Add Protein To Every Main Meal
Protein rich meals support hormone balance and assist in reducing metabolic fluctuations that may resemble patterns found in overweight women or obese women. Consistent intake improves fullness and stabilizes energy across the day. This helps the body maintain smooth metabolic rhythm.
4. Choose Healthy Fats That Support Hormones
Balanced fats aid hormone production and help regulate shifts tied to follicle stimulating hormone and reproductive age patterns. These nutrients support a more stable metabolic environment and provide long lasting energy. Including them mindfully enhances hormonal resilience.
5. Include Strength Training Two To Three Times Weekly
Strength work helps reduce abdominal fat and supports long term metabolic stability. These benefits counter internal strain sometimes associated with increased risk markers and subtle weight gain patterns. Consistent training enhances total body strength and glucose handling.
6. Use Short Walks After Meals To Improve Blood Sugar
Post meal walks encourage smoother glucose responses and reduce tendencies linked to adipose tissue accumulation. These simple routines help regulate energy swings and improve digestive comfort. Regular movement strengthens metabolic balance over time.
7. Limit Added Sugars And Refined Carbohydrates
Minimizing sugars reduces metabolic pressure that may otherwise resemble patterns seen in obese subjects. Cleaner intake helps maintain steady energy and lowers inflammatory triggers. This strengthens hormonal stability throughout the day.
8. Increase Soluble Fiber Intake Gradually
Adding fiber supports digestion and reduces metabolic fluctuations connected to pcos complications. Gradual increases help the gut adapt comfortably, improving nutrient absorption and reducing bloating. These changes strengthen metabolic steadiness across meals.
9. Stay Consistent With Stress Reduction Practices
Stress can intensify hormonal imbalance and accelerate tendencies linked to increased risk for systemic issues. Calming routines support steadier hormone rhythms and improve recovery. These patterns foster overall wellbeing in lean PCOS.
10. Monitor Progress Through Regular Blood Tests
Routine tests help detect early markers associated with heart disease, high blood pressure or deeper metabolic strain. Keeping track of internal patterns helps women address concerns before symptoms escalate. Regular results build confidence in long term management.
Example: How Small Adjustments Work Together
A lean woman might shift to low glycemic meals, add daily walks after lunch, include two strength sessions each week and review blood tests every six months.
Over time she notices fewer afternoon crashes, more stable weight around the waist and calmer cycle symptoms, which confirms that her habits are working with her hormones, not against them.
When safe weight management and insulin sensitivity improve in this way, hormones and cycles gain a more predictable rhythm, which becomes the base for understanding how lean PCOS interacts with fertility and when assisted options may be needed.
“Get Your Custom Lean PCOS Meal Plan”
Fertility Challenges In Lean PCOS And The Role Of Assisted Reproductive Technologies
Lean PCOS often involves ovulatory dysfunction influenced by androgen excess, making induce ovulation treatments more complex. Reproductive hormones shift even in normal weight women, affecting how the body responds to fertility protocols.
Understanding these hormonal patterns clarifies when assisted reproductive technologies become useful.
How Lean PCOS Affects Ovulation
In lean PCOS, ovulation may not occur regularly even when cycles appear normal. Androgen excess disrupts follicle growth, so eggs may not mature or release on time. This creates ovulatory dysfunction that lowers the chances of conception even in women with a stable body weight.
Key patterns seen in lean PCOS ovulation:
-
Follicles grow slowly or inconsistently.
-
Eggs may not reach full maturity.
-
Ovulation timing becomes unpredictable.
-
Luteal phases may be shorter or irregular.
Why Normal Weight Can Be Misleading In Fertility
Healthy weight often creates an impression that fertility should be intact. Yet ovarian function in lean PCOS does not depend on body size. Hormones can follow a PCOS pattern even when nutrition, weight and energy levels look stable.
This gap shows up through:
-
Regular looking cycles that still lack ovulation.
-
Hormone levels that shift subtly across months.
-
Follicles developing without releasing an egg.
These quiet changes explain why conception becomes difficult without an obvious cause.
When Doctors Try To Induce Ovulation
Medications are usually the first approach for lean PCOS. Doctors monitor how ovaries respond to each cycle and adjust doses as needed. Lean women often show a sharper or less predictable response, so close observation is essential.
During ovulation induction, doctors track:
-
Follicle size and growth rate
-
Hormonal markers that signal egg maturity
-
Timing of ovulation
-
Ovarian sensitivity to medication
The goal is safe and timely egg release.
How Assisted Reproductive Technologies Fit In
If several induced cycles do not lead to pregnancy, assisted reproductive technologies become the next step. These methods work by supporting egg selection, fertilisation and implantation when ovulation alone remains inconsistent.
ART options often considered include:
-
Intrauterine insemination to improve timing
-
In vitro fertilisation to work around irregular ovulation
-
Controlled ovarian stimulation for more predictable egg development
For lean PCOS, ART offers a structured pathway when hormonal patterns make natural timing unreliable.
Example: A Lean Woman Moving Toward ART
A lean woman in her early thirties may complete a few cycles of ovulation induction with no pregnancy. Follicles grow, yet ovulation remains inconsistent. After reviewing her hormone profile and ovarian response, her doctor recommends assisted reproductive technologies to increase the chances of success in each cycle.
Fertility planning in lean PCOS becomes clearer when ovulation patterns, hormonal shifts and treatment responses are monitored as closely as metabolic health.
FAQs
1. How Lifestyle Stress Influences Hormonal Balance In Lean Polycystic Ovary Syndrome?
Stress raises cortisol, which disrupts reproductive hormones and increases androgen activity. This weakens ovulation signals and makes cycles less predictable. In lean PCOS, even mild stress can shift hormones enough to intensify symptoms.
2. Why Do Some Women With Lean PCOS Struggle To Lose Weight Even With A Clean Diet?
Hormones that regulate appetite, insulin and metabolism do not respond normally in lean PCOS. Even with a clean diet, insulin resistance can slow fat use and create energy swings. The issue is hormonal signalling, not food discipline.
3. What Unique Nutrient Deficiencies Are Commonly Seen In Lean Women With PCOS?
Lean PCOS often shows lower levels of vitamin D, magnesium, omega 3 fats and B vitamins that support hormone and insulin function. These gaps can affect energy, cycles and metabolic stability even when overall diet seems balanced.
4. How Does Gut Health Shape Inflammation Patterns In Lean PCOS?
Gut imbalance can heighten inflammation, increase androgen activity and worsen insulin resistance. Changes in gut bacteria affect how nutrients are absorbed and how blood sugar behaves. A stable gut environment supports smoother hormone signalling.
5. What Long Term Heart And Metabolic Risks Should Lean PCOS Patients Monitor Beyond Insulin Issues?
Lean women with PCOS should track blood pressure, cholesterol, triglycerides and early signs of cardiovascular strain. Metabolic abnormalities can build quietly despite normal weight, so regular screening protects long term heart health.
Conclusion
A clearer picture of PCOS lean gives you room to act with intent instead of reacting to scattered symptoms. The body responds best when small adjustments are made consistently and tracked with attention, not pressure.
For example, following a high protein diet chart can provide structured guidance to maximize energy and recovery.
Each step you take builds a pattern your hormones can follow with more predictability and less strain.
When you understand how your cycles, energy and metabolism behave, the choices that support you become easier to recognise. That awareness creates a quieter, steadier path forward and helps every next decision land with more confidence than confusion.
“Join MyBalance Bite’s Weekly Hormone-Friendly Recipe Mailer”




















Leave a comment
Translation missing: en.blogs.comments.discription