Recovery from jaundice often feels slow, uncertain, and tiring, especially when food choices seem confusing or risky. What patients eat each day quietly decides whether healing moves forward or stalls.
This diet plan jaundice diet chart works because it reduces pressure on the liver while giving the body exactly what it needs to repair. Meals stay simple, digestion stays calm, and energy begins returning without forcing the system.
Patients recover faster not through shortcuts, but through consistency built into daily eating. Understanding how this structure supports healing explains why results appear sooner and feel steadier over time.
What Is Jaundice?
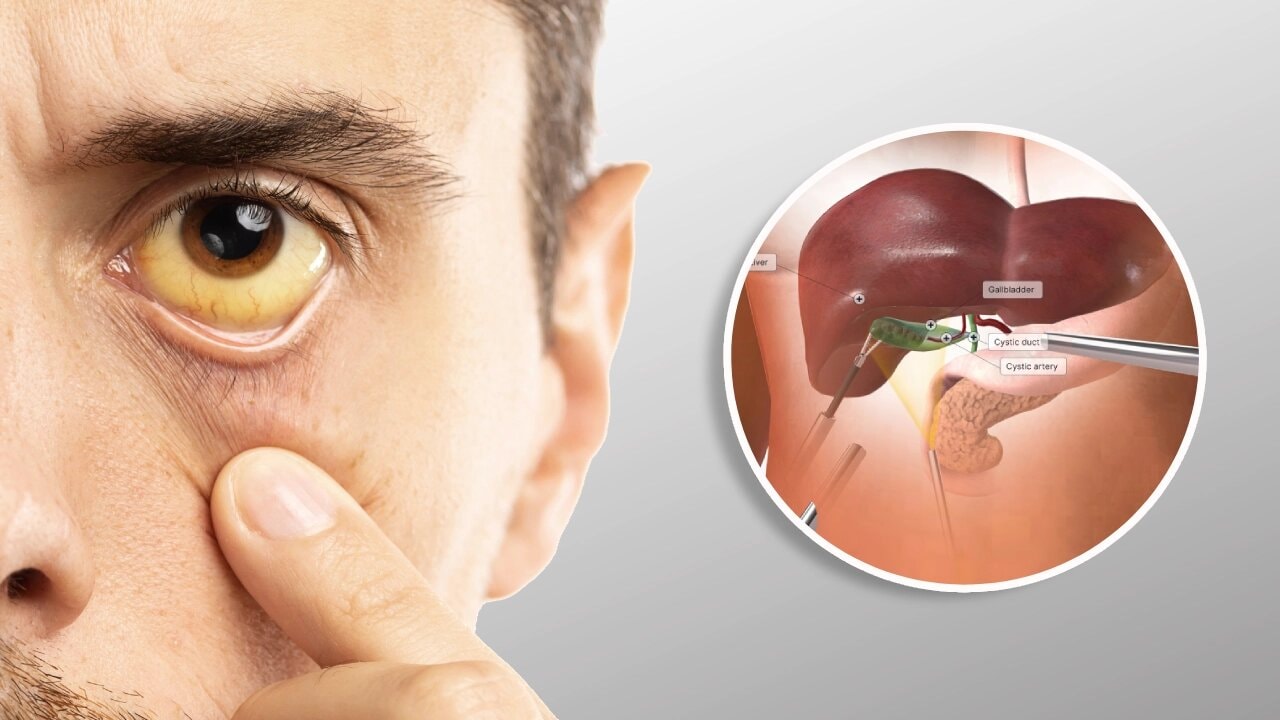
Jaundice develops when excess bilirubin builds up due to liver dysfunction, liver disease, or liver damage affecting liver cells. This disrupts digestion, weakens the immune system, and creates liver inflammation and liver stress.
Understanding how bilirubin impacts the digestive system and internal bodily tissues explains why early dietary control matters from the very start.
What Jaundice Signals Inside the Body
Bilirubin forms when old red blood cells break down. In a healthy liver, it is processed and removed through bile. When liver cells are inflamed or damaged, this process slows, allowing bilirubin to circulate longer in the blood and deposit in tissues.
How Liver Dysfunction Alters Core Functions
When liver function is compromised, several systems shift at once.
-
Bilirubin clearance slows, increasing visible symptoms
-
Bile flow weakens, affecting digestion and nutrient absorption
-
Metabolic balance drops, reducing available energy
-
Inflammatory response rises, increasing liver stress
Why Digestion and Energy Feel Different
The digestive system relies on bile to process fats and absorb nutrients. Reduced bile output makes meals feel heavier and limits how effectively internal bodily tissues receive fuel needed for repair.
How Jaundice Commonly Presents
While severity varies, most jaundice patients notice consistent patterns.
-
Yellowing of the eyes or skin
-
Darkened urine or lighter stools
-
Lower appetite with mild nausea
-
Fatigue that persists even after rest
The Immune System Connection
The liver plays a quiet but vital role in immune system regulation. When liver disease or liver damage disrupts filtration and detox pathways, recovery slows because the body remains under low-grade stress.
Why This Definition Shapes Your Diet Approach
A proper diet reduces digestive load, calms liver inflammation, and supports liver function without adding strain during recovery.
This understanding sets the stage for seeing how a poor and imbalanced diet slows liver healing in jaundice patients.
How a Poor and Imbalanced Diet Slows Liver Healing in Jaundice Patients
A poor diet increases liver stress, promotes fat accumulation, and can impair liver function during jaundice recovery. Without a healthy diet and proper diet structure, chronic inflammation worsens and essential nutrients fail to reach internal bodily tissues.
Food choices directly influence how efficiently the liver manages bilirubin and repair processes.
1. Increased Liver Stress and Delayed Bilirubin Clearance
When meals are heavy or erratic, the liver works harder to process what comes in and clear excess bilirubin. That added workload keeps liver stress high and slows visible recovery in the skin and eyes.
How it shows up
-
Appetite feels unstable across the day
-
Fatigue lingers because the body is spending energy on processing
-
Healing feels slow even when rest is adequate
2. Higher Fat Load That Weakens Digestive Efficiency
A high fat foods pattern, especially fatty foods cooked in heavy oil, is harder to break down when bile flow is already affected. This adds digestive strain and makes meals sit heavier, which can reduce intake of essential nutrients that support liver repair.
What makes fat load risky during recovery
-
Fried foods and oily gravies increase digestive effort
-
Unhealthy fats slow stomach emptying and worsen heaviness
-
Portion size matters, even when the food is otherwise healthy
3. Poor Nutrient Absorption Slowing Tissue Repair
Liver repair depends on essential nutrients reaching the cells that are rebuilding. When digestion is weak or food quality is low, absorption drops, and internal bodily tissues do not get steady fuel for recovery.
Essential nutrients most linked to recovery
-
Protein for tissue rebuilding
-
Vitamins and minerals from whole foods
-
Fluids and electrolytes for cellular balance
4. Dehydration and Electrolyte Imbalance
Hydration affects circulation, digestion, and nutrient movement. Low fluids make it harder to maintain electrolyte balance, which can worsen weakness and slow recovery rhythm.
Common dehydration triggers
-
Low water intake due to nausea
-
Excess tea or coffee replacing fluids
-
Sugary drinks that worsen fluid balance
5. Inflammation Triggered by Fried and Processed Foods
Processed foods, highly processed foods, and fried foods increase inflammatory load. This can aggravate liver inflammation and make the liver’s repair cycle less efficient, especially while clearing bilirubin.
Examples
-
Packaged snacks and instant foods
-
Bakery items made with refined fats
-
Sugary foods combined with oil, like desserts
6. Weakened Immunity Increasing Recovery Time
The immune system relies on steady nutrition and liver support to regulate inflammation and healing. When diet quality drops, immunity weakens, recovery takes longer, and fatigue becomes harder to shake off.
What supports immunity during recovery
-
Regular meals
-
Clean, digestible foods
-
Adequate fluids and rest support
A clearer diet structure is what turns this damage control into steady healing, which is exactly why the next step focuses on a diet plan for jaundice patients built for liver recovery and strength.
Diet Plan for Jaundice Patients Focused on Liver Recovery and Strength
A structured jaundice diet plan supports liver recovery by reducing digestive load while improving liver repair and liver regeneration. The right proper diet helps support liver function, restores strength, and promotes liver health without triggering further stress.
This approach balances nourishment with tolerance during active healing.
| Meal Time | Vegetarian Option (Portion & Calories) | Non-Vegetarian Option (Portion & Calories) | Vegan Option (Portion & Calories) |
|---|---|---|---|
| Early Morning | Warm water + 1 fruit portion (papaya or apple), 100 g, ~60 kcal | Same as vegetarian | Same as vegetarian |
| Breakfast | Oats porridge with low fat milk, 1 bowl, ~220 kcal. For a balanced meal, consider adding some of the best fruits for PCOS to help support hormone balance. | Oats porridge with low fat milk + 1 boiled egg white, ~260 kcal | Oats porridge with water or almond milk, 1 bowl, ~200 kcal |
| Mid-Morning | Fruit bowl (citrus fruits or watermelon), 150 g, ~70 kcal | Same as vegetarian | Same as vegetarian |
| Lunch | Steamed rice or brown rice (1 cup), sautéed vegetables (1 cup), curd (½ cup), ~380 kcal | Steamed rice (1 cup), boiled chicken or fish (80 g), vegetables (1 cup), ~420 kcal | Steamed rice (1 cup), lentils or tofu (80 g), vegetables (1 cup), ~400 kcal |
| Evening Snack | Herbal tea + roasted chana (30 g), ~120 kcal | Herbal tea + roasted chana (30 g), ~120 kcal | Herbal tea + roasted chana (30 g), ~120 kcal |
| Dinner | Soft roti (1 medium), vegetable curry (1 cup), ~260 kcal | Soft roti (1 medium), grilled fish or chicken (70 g), vegetables, ~300 kcal | Soft roti (1 medium), tofu or lentil curry (1 cup), ~280 kcal |
| Bedtime | Warm low fat milk (1 cup), ~100 kcal | Warm low fat milk (1 cup), ~100 kcal | Warm plant milk (1 cup), ~90 kcal |
This table shows how meals stay simple, portion controlled, and evenly spread to avoid liver stress while meeting daily energy needs. Calories remain moderate, digestion stays light, and nutrient flow stays steady across the day.
Once the structure is clear, the next focus shifts to identifying which fresh fruits and vegetables actively support liver healing during jaundice recovery.
Must Have Fresh Fruits and Vegetables That Aid Liver Healing in Jaundice
Fresh fruits and vegetables provide essential nutrients that support liver health while aiding liver detoxification. Citrus fruits, leafy greens, and antioxidant rich produce supply phenolic acid and fiber that protect liver cells and improve digestion.
These are among the best foods and right foods during jaundice recovery.
1. Papaya
Papaya is gentle on digestion and fits well when the stomach feels sensitive. Its soft texture makes it easy to eat even when appetite is inconsistent.
Best way to take it
-
100 to 150 g, mid morning or evening
2. Apple
Apple supports digestion through fiber and works well as a steady snack. It is easy to portion and does not overload the stomach.
Best way to take it
-
1 small apple, peeled if needed
3. Banana
Banana provides quick energy without feeling heavy. It suits low appetite phases and can help maintain daily calorie intake without strain.
Best way to take it
-
1 small banana, mid morning or post lunch
4. Watermelon
Watermelon supports hydration and feels light on the digestive system. It helps when the mouth feels dry or when heavy meals feel difficult.
Best way to take it
-
1 bowl, 150 g, early afternoon
5. Orange
Orange is one of the useful citrus fruits for vitamin support, but it should be taken in modest portions to avoid acidity sensitivity.
Example
-
1 orange after breakfast, not on an empty stomach — if you're stuck in a weight loss plateau, consider reviewing strategies to keep making progress.
6. Pomegranate
Pomegranate offers antioxidants and phenolic acid that support liver cells during recovery. It works best as a small portion, since very large servings can feel heavy.
Best way to take it
-
½ cup seeds, mid morning
7. Carrot
Carrot provides vitamins that support recovery and is easier to digest when lightly cooked. It fits well as part of a simple meal plate.
Best way to take it
-
Steamed or boiled, 1 cup
8. Beetroot
Beetroot supports liver detoxification and contains phenolic acid, but it should be introduced in small portions. Light cooking improves tolerance.
Best way to take it
-
Boiled, ½ cup, with lunch
9. Bottle Gourd (Lauki)
Bottle gourd is one of the cleanest vegetables for jaundice recovery because it is watery, light, and easy on digestion. It supports fluid balance without heaviness.
Best way to take it
-
Cooked sabzi, 1 cup, lunch or dinner
10. Spinach
Spinach is a strong leafy greens option for essential nutrients. It should be cooked well for better digestion and smoother absorption.
Get a Customized Fruit & Meal Plan for Your Healing Goals
Best way to take it
-
Cooked, 1 cup, paired with rice or roti
How to use this list
-
Keep portions light, spread them across the day
-
Prefer whole fruits over juices for fiber support
-
Choose soft textures when appetite is low
-
Pair meals with fluids, including coffee and herbal teas, only if tolerated
Once these fruits and vegetables are in place, the next focus becomes choosing healthy fats that support liver healing without slowing digestion.
Healthy Fats That Are Safe During Jaundice
Not all fats harm recovery. Healthy fats support energy needs without worsening liver stress, unlike unhealthy fats, trans fats, or saturated and trans fats that strain digestion.
Choosing the correct fat sources helps avoid fatty foods while still supporting healing and hormone balance during jaundice recovery.
Why fats still matter during recovery
Fat supports hormones, cell repair, and steady energy. When portions stay small, the body can use fat without overloading digestion. The goal is controlled intake, not elimination.
Healthy fats that are usually well tolerated
-
Olive oil, 1 teaspoon added after cooking
-
Ground flaxseed, 1 teaspoon mixed into oats or porridge
-
Chia seeds, 1 teaspoon soaked and added to fruit
-
Walnuts, 2 to 3 pieces, only if digestion feels stable
-
Almonds, 4 to 6 soaked, taken mid morning
Example
A bowl of oats with 1 teaspoon ground flaxseed gives gentle fat support without feeling heavy.
Fats to avoid during jaundice recovery
-
Trans fats from bakery items and packaged snacks
-
Saturated and trans fats from fried foods and commercial gravies
-
Fatty foods like deep fried snacks, creamy sauces, and rich desserts
Portion rules that keep fats safe
-
Start small, 1 teaspoon oil or a few nuts at a time
-
Use fats as add-ons, not the base of the meal
-
Avoid frying, choose steaming, boiling, or light cooking
-
Watch response, heaviness after meals means the portion was too high
Once fat choices are clear, the next step is making everyday decisions easier through a foods to eat and foods to avoid checklist built for jaundice recovery.
Foods to Eat and Avoid Checklist for Jaundice Recovery
A clear eat and avoid approach simplifies food decisions during jaundice recovery. Identifying foods to eat such as whole grains, lean proteins, low fat dairy products, and essential foods prevents confusion, while knowing foods to avoid limits processed foods, sugary foods, and high fat foods.
This checklist supports consistent dietary discipline.
| Food Area | Choose These (Foods to Eat) | Limit or Avoid These (Foods to Avoid) |
|---|---|---|
| Grains | Brown rice, oats, soft roti, simple whole grains | Refined grains, white bread, deep fried snacks |
| Protein Sources | Dal, tofu, egg whites, boiled chicken or fish | Fatty meats, organ meats, processed protein |
| Dairy | Low fat milk, curd, low fat dairy products | Full fat milk, cream, cheese |
| Fruits | Fresh fruits and vegetables, papaya, apple, citrus fruits | Fruit juices with added sugar, canned fruits |
| Vegetables | Steamed vegetables, sautéed vegetables, leafy greens | Fried vegetables, canned vegetables |
| Fats | Healthy fats in small portions, olive oil, nuts | High fat foods, trans fats, saturated and trans fats |
| Snacks & Drinks | Water, herbal teas, light homemade snacks | Sugary foods, sugary drinks, packaged snacks |
| Cooking Style | Boiling, steaming, light sauté | Deep frying, reused oil, heavy gravies |
This layout allows the eye to compare choices instantly while keeping decisions calm and practical. With clarity in what to eat and what to avoid, the next step is understanding the common diet mistakes jaundice patients should avoid during recovery.
See Your Personalized Weekly Grocery List
Common Diet Mistakes Jaundice Patients Should Avoid
Many jaundice patients unknowingly slow healing by consuming processed foods, fruit juices, unhealthy fats, or sugary drinks that increase liver stress. Ignoring hydration, overeating, or returning to alcohol too early can impair liver function and extend recovery.
These mistakes often appear harmless but carry lasting consequences.
1. Eating Fried or Oily Foods Too Early
Fried foods increase digestive load when the liver is still repairing. Even small portions can trigger heaviness and delay progress.
Why it matters
-
Adds high fat foods that strain digestion
-
Increases liver stress during active recovery
Example
A single plate of fried snacks can make the next meal feel harder to tolerate.
2. Skipping Meals Due to Low Appetite
Skipping meals reduces energy intake and disrupts steady nourishment. The liver still needs essential nutrients, even when appetite is limited.
What helps
-
Small, frequent meals
-
Soft, easy foods that feel light
3. Avoiding All Fats Instead of Choosing Healthy Fats
Cutting fats completely can reduce calorie intake and slow strength recovery. Healthy fats in small portions support repair without overloading digestion.
Better approach
-
Use 1 teaspoon olive oil
-
Add a few soaked nuts if tolerated
4. Relying Only on Fruit Juices Instead of Whole Fruits
Fruit juices spike sugar faster and reduce fiber intake. Whole fruits support digestion and provide steadier energy.
What to choose
-
Papaya, apple, banana
-
Citrus fruits in moderate portions
5. Consuming Processed or Packaged Foods
Processed foods and highly processed foods often contain trans fats, refined sugar, and additives that disrupt recovery. These foods increase inflammation and delay healing rhythm.
Common triggers
-
Packaged snacks
-
Instant noodles and ready meals
6. Ignoring Hydration and Fluid Intake
Hydration supports circulation and digestion. Low fluids increase weakness and make recovery feel slower.
Hydration supports
-
Better digestion
-
Stable energy across the day
7. Overeating in the Name of Gaining Strength
Large meals increase digestive stress, even when the food itself is healthy. Recovery improves with steady intake, not heavy portions.
Portion rule
-
Stop when you feel comfortably full, not stuffed
8. Resuming Alcohol Intake Before Full Liver Recovery
Alcohol burdens the liver and can reverse recovery gains. Even small amounts can increase liver stress and prolong symptoms.
Clear guidance
-
Avoid alcohol until liver function normalizes and your doctor clears it
Once these mistakes are understood, long term recovery becomes easier to protect through steady lifestyle practices that maintain liver health after jaundice.
Long Term Lifestyle Practices for Jaundice Maintenance

Long term jaundice maintenance focuses on protecting a healthy liver by stabilizing blood sugar, supporting digestion, and preventing fat buildup.
Following frequent meals, choosing liver friendly nutrients, limiting refined sugar, caffeine alcohol, and excessive alcohol consumption reduces relapse risk and conditions like nonalcoholic fatty liver disease. Consistent choices help sustain recovery beyond symptoms.
1. Following a Consistent Balanced Diet
A balanced diet built around whole foods supports steady blood sugar and reduces fat accumulation. It also keeps essential nutrients flowing to repair systems that are still stabilizing after jaundice recovery.
What this looks like daily
-
Include fruits and vegetables with each main meal
-
Keep protein steady, not occasional
-
Use simple cooking methods that protect digestion
2. Prioritizing Regular and Frequent Meals
Frequent meals reduce sudden hunger spikes and prevent overeating later. This pattern supports digestion and keeps energy more stable through the day.
A practical rhythm
-
3 meals with 2 light snacks
-
Smaller portions, spaced evenly
Example
A mid morning fruit portion and a light evening snack often prevent heavy dinners.
3. Limiting Alcohol and Caffeine Intake Long Term
Limiting caffeine alcohol protects liver cells from renewed stress. Avoiding excessive alcohol consumption helps keep liver function steady and reduces the chance of recurring inflammation.
Clear rule
-
Keep alcohol off the routine, not just off the week
4. Choosing Whole, Fresh Foods Over Processed Options
Highly processed foods add preservatives, refined fats, and sugar that can disrupt liver stability. Limiting canned vegetables and smoked foods keeps the diet cleaner without needing strict restrictions.
Better cooking choices
-
Sautéed vegetables
-
Simple soups and dals
-
Freshly prepared meals
5. Maintaining Hydration to Support Digestion
Hydration aids digestion and supports daily detox work without stressing the liver. Limiting sugary drinks helps prevent unnecessary blood sugar spikes that can affect energy and appetite.
Simple hydration cues
-
Clear urine most of the day
-
Water with each meal and snack
6. Including Gentle Physical Activity for Metabolic Support
Gentle activity supports circulation and helps prevent fat buildup without exhausting recovery reserves. The goal is consistency, not intensity.
Low strain options
-
Walking after meals
-
Light stretching
-
Short morning mobility routines
7. Monitoring Liver Health Through Periodic Checkups
Periodic monitoring helps track liver dysfunction early, before symptoms return. Follow-ups make maintenance more precise, especially if fatigue or appetite changes reappear.
What to track
-
Liver enzymes as advised
-
Appetite patterns and energy stability
8. Avoiding Long-Term Reliance on Fried and Fatty Foods
Limiting fatty foods supports digestion and reduces fat accumulation. A stable base built on low fat milk, brown rice, brown rice oats, lean proteins protein, and lean proteins tofu supports long term liver stability without dietary stress.
When these habits become routine, the final step is answering the common questions people still carry about jaundice recovery and daily food choices.
FAQs
1. Can Herbal Teas Be Safely Included During Jaundice Recovery?
Yes, herbal teas can be included if taken in moderation and tolerated well. Options like ginger or chamomile support digestion and hydration without adding strain. Avoid strong or concentrated blends, and treat herbal teas as support, not a replacement for meals or fluids.
2. Why Are Fried Foods Considered Risky Even After Symptoms Improve?
Fried foods increase digestive load and liver stress, even when visible symptoms reduce. The liver may still be healing internally, and heavy fats can slow recovery or trigger fatigue, heaviness, or poor appetite during this phase.
3. How Long Should a Diet for Jaundice Be Followed After Recovery Begins?
A jaundice-focused diet should continue for several weeks after symptoms improve. Liver recovery takes longer than symptom relief, so maintaining a structured diet helps stabilize function before gradually returning to normal eating.
4. How Does a Balanced Diet Help Prevent Weakness After Jaundice?
A balanced diet provides steady energy, protein for repair, and nutrients that support digestion. This prevents sudden fatigue, muscle weakness, and appetite swings that often follow jaundice if meals are irregular or poorly planned.
5. Are There Any Essential Foods That Support Appetite When Eating Feels Difficult?
Yes. Soft fruits like papaya and banana, light grains, soups, and curd are easier to tolerate. These essential foods provide calories and nutrients without overwhelming digestion when appetite is low.6. What Are Considered the Best Foods to Rebuild Strength After Jaundice Recovery?
The best foods include whole grains, lean proteins, fresh fruits and vegetables, and low fat dairy. These support gradual strength rebuilding without overloading the liver or digestive system.
7. Which Foods to Avoid Even After Liver Function Starts Normalizing?
Foods to avoid include fried items, processed foods, sugary snacks, alcohol, and heavy fatty foods. Even after liver function improves, these can slow full recovery if reintroduced too early.
Conclusion
Recovery from jaundice improves when food stops adding pressure and starts supporting the body’s repair work. This diet plan offers that shift by giving the liver a steady rhythm instead of constant adjustment.
What matters now is consistency. Follow the structure, respect portions, and listen to how your body responds after each meal. Small daily choices create the conditions where recovery continues quietly and strength returns without forcing the process.
Connect With a Nutrition Expert to Plan Your Next Steps




















Leave a comment
Translation missing: en.blogs.comments.discription