Eating should feel safe, but with ulcerative colitis it often feels like a risk you have to calculate. One wrong meal can change how your entire day unfolds.
This is why random food advice fails. When symptoms are unpredictable, clarity matters more than restriction.
This diet plan ulcerative colitis patients rely on brings structure to eating when tolerance feels uncertain, helping daily digestion stay steadier and more predictable.
What Is Ulcerative Colitis and How It Leads to Inflammatory Bowel Disease?
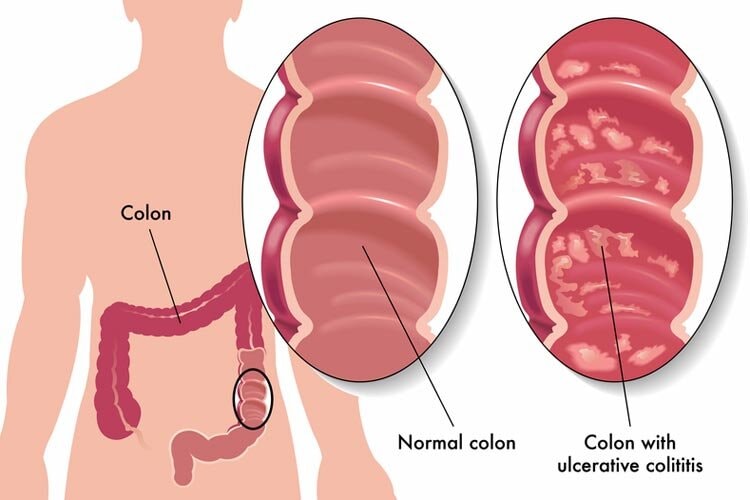
Ulcerative colitis is a chronic inflammatory bowel disease that affects the digestive tract, specifically the colon lining. Over time, persistent inflammation can overlap with broader inflammatory bowel disease conditions, including Crohn's disease.
In some people, complications extend beyond digestion and may intersect with digestive and kidney diseases. Understanding this foundation clarifies why dietary decisions matter at every stage of the condition.
What’s happening inside the digestive tract
-
The colon lining becomes fragile and less efficient at absorption.
-
Normal food volume can trigger urgency or cramping.
-
Fermentation increases, intensifying gas and discomfort.
-
Nutrient uptake becomes inconsistent during active phases.
These shifts explain why tolerance can vary from one day to the next.
How inflammatory bowel disease connects ulcerative colitis and Crohn’s disease
Inflammatory bowel disease is a medical category, not a single condition. Ulcerative colitis and Crohn's disease fall under the same umbrella because both involve immune-driven inflammation, yet they behave differently.
Ulcerative colitis remains confined to the colon, while Crohn’s disease can affect multiple areas of the digestive tract. This distinction influences symptom patterns and dietary tolerance.
Why effects can extend beyond digestion
Chronic inflammation rarely stays isolated. Ongoing stress on the digestive system can affect hydration, electrolyte balance, and kidney function in some individuals.
This explains why ulcerative colitis is sometimes discussed alongside digestive and kidney diseases rather than as a condition limited to the gut.
Example
A meal with raw vegetables may feel manageable during a calm phase. The same meal can trigger urgency or pain during inflammation. The difference lies in the condition of the colon lining, not the food itself.
Once this internal instability is clear, the role of diet in worsening symptoms or supporting healing becomes easier to see.
How a Poor Diet Can Worsen Symptoms and Delay Healing?

A poor diet can worsen symptoms by irritating the digestive tract during active disease phases. Foods that aggravate symptoms often intensify abdominal pain, digestive symptoms, and UC symptoms, making ulcerative colitis flare ups harder to control.
When eating habits consistently trigger inflammation, symptoms become worse and ulcerative colitis flare episodes last longer than necessary.
What poor diet looks like in real life
Poor diet is rarely one “bad food.” It is a pattern that keeps the gut on edge.
-
Large meals that overload digestion during active disease
-
Frequent fried, greasy, or heavily seasoned choices
-
High sugar intake that fuels irritation and unstable stools
-
Low fluid intake that worsens cramping and fatigue
Why symptoms escalate instead of settling
When the digestive tract is inflamed, the colon lining reacts faster to volume, fat, and rough textures. That reaction increases urgency, amplifies abdominal pain, and keeps digestive symptoms cycling.
Over time, the body spends more energy coping with irritation than repairing tissue, so symptoms worse becomes the new baseline.
What delayed healing actually means
Delayed healing shows up as repeated flare patterns, lower appetite, and shrinking food tolerance. It can also mean nutrient gaps because meals become limited and inconsistent, especially when people skip foods that feel “unsafe.”
Example
A simple dinner of baked sweet potatoes and soft protein may feel calm on the gut, while a fried snack or spicy meal the same day can trigger urgency within hours. The contrast is not willpower, it is how inflammation responds to stress.
Once you see how irritation prolongs a flare, structured diet plans start to feel less like rules and more like control.
Structured Diet Plans Designed to Manage Ulcerative Colitis
A structured approach to an ulcerative colitis diet plan helps control ulcerative colitis by reducing guesswork around meals. Rather than random restriction, a clear diet plan ulcerative colitis patients follow supports nutritional therapies and dietary guidance.
This structure allows an effective UC diet to stabilize digestion and support consistent symptom management over time.
1. Mediterranean Diet
The Mediterranean diet emphasizes healthy fats, olive oil, omega 3 fatty acids, and omega fatty acids that support anti-inflammatory balance. It prioritizes whole grains, fruits and vegetables, and other nutritious foods that nourish without overwhelming digestion.
For ulcerative colitis management, this pattern supports gut stability while maintaining long-term nutritional adequacy.
| Meal | Vegetarian | Non-Vegetarian | Vegan |
|---|---|---|---|
| Breakfast | Oats 70 g, milk 250 ml, fruit (450 kcal) | Eggs 3, oats 50 g (440 kcal) | Oats 70 g, soy milk, fruit (430 kcal) |
| Mid-Morning | Greek yogurt 200 g (200 kcal) | Greek yogurt 200 g (200 kcal) | Soy yogurt 200 g (190 kcal) |
| Lunch | Brown rice 110 g, paneer 140 g (600 kcal) | Brown rice 110 g, chicken 170 g (580 kcal) | Brown rice 110 g, lentils 200 g (560 kcal) |
| Pre-Workout | Banana, coffee (120 kcal) | Banana, coffee (120 kcal) | Banana, coffee (120 kcal) |
| Post-Workout | Whey protein 1 scoop (120 kcal) | Whey protein 1 scoop (120 kcal) | Plant protein 1 scoop (120 kcal) |
| Dinner | Whole wheat roti 3, vegetables (450 kcal) | Whole wheat roti 3, fish 150 g (470 kcal) | Whole wheat roti 3, chickpea curry (450 kcal) |
2. Low FODMAP Diet
The low FODMAP diet was developed for irritable bowel syndrome but often benefits ulcerative colitis patients sensitive to certain foods. By reducing fermentable carbohydrates, this approach helps identify food triggers that cause bloating, gas, and trigger symptoms.
It works best as a structured elimination and reintroduction strategy rather than a permanent restriction.
| Meal | Vegetarian | Non-Vegetarian | Vegan |
|---|---|---|---|
| Breakfast | Rice flakes 40 g, lactose-free milk 150 ml (280 kcal) | Rice flakes 40 g, egg omelette 1 (300 kcal) | Rice flakes 40 g, almond milk 150 ml (290 kcal) |
| Mid-Morning | Banana ½ (90 kcal) | Banana ½ (90 kcal) | Banana ½ (90 kcal) |
| Lunch | White rice 1 cup, zucchini 1 cup (380 kcal) | White rice 1 cup, grilled chicken 100 g (430 kcal) | White rice 1 cup, firm tofu 100 g (410 kcal) |
| Evening Snack | Rice cakes 2 with peanut butter 1 tsp (180 kcal) | Same as veg (180 kcal) | Same as veg (180 kcal) |
| Dinner | Potatoes 1 cup boiled, carrots 1 cup (340 kcal) | Potatoes 1 cup, fish 100 g (390 kcal) | Potatoes 1 cup, tempeh 80 g (380 kcal) |
3. Low Residue Diet During Flares
A low residue approach reduces digestive workload during flares by limiting foods high in insoluble fiber. It emphasizes low fiber fruits, white rice, brown rice in moderation, and starchy vegetables while avoiding high fiber foods.
This helps calm insoluble fibre irritation when the gut is inflamed and vulnerable.
| Meal | Vegetarian | Non-Vegetarian | Vegan |
|---|---|---|---|
| Breakfast | White toast 2 slices, butter 1 tsp (260 kcal) | White toast 2 slices, egg whites 2 (280 kcal) | White toast 2 slices, plant margarine 1 tsp (270 kcal) |
| Mid-Morning | Applesauce ½ cup (100 kcal) | Applesauce ½ cup (100 kcal) | Applesauce ½ cup (100 kcal) |
| Lunch | White rice 1 cup, mashed carrots ½ cup (350 kcal) | White rice 1 cup, chicken breast 100 g (420 kcal) | White rice 1 cup, silken tofu 100 g (400 kcal) |
| Evening Snack | Crackers 4–5 (150 kcal) | Same as veg (150 kcal) | Same as veg (150 kcal) |
| Dinner | Mashed potatoes 1 cup (320 kcal) | Mashed potatoes 1 cup, fish 100 g (380 kcal) | Mashed potatoes 1 cup, soy yogurt 100 g (360 kcal) |
4. Elimination Diet Based on Trigger Foods
An elimination diet focuses on identifying trigger foods through controlled removal and reintroduction. Tracking following foods and reactions helps isolate problem ingredients without unnecessary restriction.
This approach relies on observation rather than assumptions and supports individualized tolerance patterns that differ widely among patients.
| Meal | Vegetarian | Non-Vegetarian |
Vegan 1 Month Diet Plan for Weight Loss |
|---|---|---|---|
| Breakfast | Plain oats 40 g, water (250 kcal) | Plain oats 40 g, egg whites 2 (270 kcal) | Plain oats 40 g, almond milk 150 ml (260 kcal) |
| Mid-Morning | Pear ½ (80 kcal) | Pear ½ (80 kcal) | Pear ½ (80 kcal) |
| Lunch | White rice 1 cup, tolerated vegetable 1 cup (380 kcal) | White rice 1 cup, grilled turkey 100 g (430 kcal) | White rice 1 cup, tofu 100 g (410 kcal) |
| Evening Snack | Rice crackers 3 (120 kcal) | Same as veg (120 kcal) | Same as veg (120 kcal) |
| Dinner | Quinoa ¾ cup, tolerated vegetables (340 kcal) | Quinoa ¾ cup, fish 100 g (400 kcal) | Quinoa ¾ cup, lentils ½ cup (390 kcal) |
5. Specific Carbohydrate Diet
The specific carbohydrate diet limits complex sugars and emphasizes proper nutrition through easily digestible carbohydrates. By restricting sugar and electrolyte salts that may ferment in the gut, this approach aims to reduce inflammation drivers.
Its effectiveness varies and requires careful planning to maintain balance.
| Meal | Vegetarian | Non-Vegetarian | Vegan |
|---|---|---|---|
| Breakfast | Homemade yogurt 150 g, honey 1 tsp (220 kcal) | Same as veg (220 kcal) | Coconut yogurt 150 g (240 kcal) |
| Mid-Morning | Banana 1 small (100 kcal) | Banana 1 small (100 kcal) | Banana 1 small (100 kcal) |
| Lunch | Cooked vegetables 1 cup, paneer 80 g (380 kcal) | Cooked vegetables 1 cup, chicken 100 g (420 kcal) | Cooked vegetables 1 cup, nut butter 1 tbsp (400 kcal) |
| Evening Snack | Boiled carrots 1 cup (90 kcal) | Same as veg (90 kcal) | Same as veg (90 kcal) |
| Dinner | Zucchini noodles 1½ cups, olive oil 1 tsp (300 kcal) | Zucchini noodles, fish 100 g (360 kcal) | Zucchini noodles, tofu 100 g (350 kcal) |
How to Know Which Diet Plan Fits Your Current Phase
Ulcerative colitis does not behave the same way every day. Symptoms rise and settle in phases, and diet works best when it adjusts with those changes rather than fighting them.
During flare phases
-
Digestion needs rest, not variety
-
Portions matter more than food diversity
-
Softer textures reduce strain on the colon
-
Simplicity supports healing better than experimentation
During remission or stable phases
-
Nutrient rebuilding becomes the priority
-
Food variety can expand gradually
-
Healthy fats and balanced meals support resilience
-
Structure prevents accidental trigger stacking
This distinction helps users choose a diet plan with confidence instead of second-guessing every meal.
How to Read Food Reactions Without Overreacting
Not every symptom means a food is harmful. In ulcerative colitis, timing and quantity often matter more than the ingredient itself.
What usually signals a real trigger
-
Symptoms appear consistently within a few hours
-
Reactions repeat across multiple meals
-
Smaller portions still cause discomfort
What often reflects temporary sensitivity
-
One-off reactions during flares
-
Discomfort only after large portions
-
Symptoms linked to stress or rushed eating
This perspective prevents unnecessary restriction while still protecting symptom control.
A Simple Way to Apply Everything Without Overthinking
Most progress comes from reducing friction, not perfect execution.
-
Eat fewer foods more consistently
-
Adjust portions before cutting ingredients
-
Change texture before changing the food itself
-
Track patterns, not isolated meals
This approach keeps decisions calm and sustainable.
Once diet choices feel clearer and less reactive, the next layer is how those foods are handled before they reach the plate. The way meals are cooked, combined, and textured often decides whether digestion feels calm or strained.
If planning meals feels overwhelming, MyBalanceBite helps turn nutrition guidance into everyday eating habits that fit real digestive needs.
Food Preparation Methods That Improve Digestive Tolerance
Food preparation affects tolerance as much as food choice itself. Simple techniques like steaming, slow cooking, and pureeing reduce irritation. Knowing how to prepare meals using options like smooth peanut butter, almond milk, or gentle fats can lower stress on digestion.
Thoughtful food preparation supports absorption while reducing mechanical strain.
Why preparation changes tolerance
When the gut is sensitive, texture and density matter. Soft foods move through the digestive tract with less friction, and gentle cooking lowers the burden of breaking down meals.
Techniques that make meals easier to tolerate
-
Steam vegetables until soft, then mash or blend if needed
-
Slow cook lentils, rice, and proteins until they are tender
-
Puree soups and dals to reduce rough texture
-
Peel and cook fruits, then use them as soft portions
Smart ingredient swaps that keep meals gentle
-
Use almond milk instead of heavy dairy in porridges and smoothies
-
Choose smooth peanut butter in small amounts for easy calories
-
Add gentle fats like a teaspoon of olive oil after cooking
Example
A raw salad can feel sharp on the gut, while the same vegetables steamed and blended into a soup often feel calmer. The ingredients stay similar, but the texture changes the outcome.
Once preparation becomes part of the plan, it is easier to understand why certain foods should be limited or avoided for steadier symptom control.
Foods to Limit or Avoid for Better Symptom Control
Certain foods consistently disrupt digestion in ulcerative colitis, especially during flares. Processed foods, fried foods, sugary foods, red meat, and processed meats commonly aggravate inflammation.
Learning when to avoid spicy foods and similar irritants helps stabilize digestion and reduce unpredictable symptom spikes.
1. High Fiber and Raw Vegetables
Foods high in insoluble fiber such as raw vegetables and brussels sprouts can irritate the colon lining during inflammation. These foods increase stool bulk and mechanical stress, making digestion more difficult when the gut is already inflamed.
What to watch for
-
Crunchy salads, raw sprouts, and large bowls of mixed vegetables
-
Skin-on vegetables that increase roughness in the gut
Practical adjustment
Cook vegetables until soft, then chop fine or blend into soups.
2. Spicy and Heavily Seasoned Foods
Spicy foods stimulate the digestive tract and may increase gut sensitivity. For people with ulcerative colitis, spices can intensify irritation and worsen bowel urgency, especially during flare periods.
What to watch for
-
Chili-heavy gravies, spicy pickles, and masala overload
-
High heat seasoning layered across multiple meals
Practical adjustment
Use mild herbs, salt, and gentle flavoring, then increase slowly during stable phases.
3. Dairy Products With Lactose
Cow's milk and lactose-containing dairy products often cause bloating and discomfort. Lactose intolerance is common during inflammation, making dairy a frequent contributor to digestive distress.
What to watch for
-
Milk-based shakes, paneer-heavy meals, and creamy sauces
-
Symptoms that appear soon after dairy intake
Practical adjustment
Try lactose-free options or small portions of fermented dairy if tolerated.
4. Fried and High Fat Foods
High fat foods slow digestion and increase inflammatory responses. Fried foods are particularly problematic because they stress bile processing and irritate the intestinal lining.
What to watch for
-
Deep-fried snacks, fast food, and oily gravies
-
Heavy meals late at night
Practical adjustment
Choose grilled, baked, steamed, or sautéed with measured fat.
5. Caffeinated Beverages
Caffeine stimulates bowel movement and increases urgency. For many people with ulcerative colitis, this stimulation worsens diarrhea and cramping.
What to watch for
-
Coffee on an empty stomach
-
Multiple cups close together
Practical adjustment
Reduce gradually, and shift to low-caffeine options if needed.
6. Alcoholic Drinks
Alcohol disrupts the gut barrier and increases inflammation. Even small amounts can intensify symptoms during active disease phases.
What to watch for
-
Drinking during flares or dehydration
-
Sugary mixed drinks that add extra irritation
Practical adjustment
Avoid during active symptoms, and keep decisions aligned with medical guidance.
7. Carbonated Beverages
Carbonated beverages introduce gas into the digestive system, increasing bloating and discomfort. They also often contain sugars or additives that worsen symptoms.
What to watch for
-
Soda, sparkling drinks, and fizzy mixers
-
Gas and bloating that builds after meals
Practical adjustment
Replace with water, diluted juice, or oral rehydration fluids when needed.
8. Added Sugars and Sweetened Foods
Sugary foods promote fermentation and inflammation in the gut. Excess sugar intake often worsens digestive instability and flare severity.
What to watch for
-
Sweets, desserts, and sugar-heavy snacks
-
Sugary drinks that spike symptoms quickly
Practical adjustment
Use small portions, and pair with a meal to reduce gut shock.
9. Processed and Packaged Foods
Processed foods and processed meats contain additives that irritate the gut lining. These foods also displace nutrient-dense options that support healing.
What to watch for
-
Packaged snacks, ready meals, and processed meats
-
Meals built around preservatives and emulsifiers
Practical adjustment
Keep staples simple, and aim for home-cooked meals most days.
10. Artificial Sweeteners and Sugar Alcohols
Artificial sweeteners can cause bloating and diarrhea. Sugar alcohols are poorly absorbed and often trigger digestive upset in sensitive individuals.
What to watch for
-
“Sugar-free” products, gums, and diet drinks
-
Bloating that feels sharp and sudden
Practical adjustment
Check labels, and treat sweeteners like a trigger test, not a free pass.
Why these foods cause trouble
During inflammation, the colon lining reacts faster to rough texture, heavy fat, and additives. Some foods increase gut movement, some increase gas, and some irritate the lining directly. The result is often urgency, cramping, and looser stools.
How to use this list without over-restricting
Treat it as a signal system, not a lifetime ban.
-
Limit more strictly during flare periods
-
Test portions before removing an entire food group
-
Track timing of symptoms, not just the ingredient
-
Focus on texture and fat level, not just “healthy” labels
Example
A grilled meal with simple seasoning may sit well, while the same meal fried or heavily spiced can trigger urgency within hours. The ingredient looks similar, but the preparation changes how the gut responds.
Once you know what commonly triggers symptoms, the next step is learning how to manage ulcerative colitis with a diet plan that stays stable in real life.
How to Manage Ulcerative Colitis With the Right Diet Plan?
Managing ulcerative colitis requires more than avoiding trigger foods. A structured approach helps people with UC reduce symptoms, prevent flare ups, and regain consistency. When meals support digestion instead of stressing it, long-term control becomes realistic rather than reactive.
This is where planning replaces trial-and-error eating.
What “the right plan” actually means
The right plan is the one your gut can repeat. It supports energy, reduces symptom spikes, and stays flexible across flare and stable phases.
Core principles that make a diet plan work
-
Keep meals predictable in timing and portion size
-
Choose soft textures during sensitive periods
-
Build calories from simple carbs, proteins, and gentle fats
-
Add variety slowly, one change at a time
-
Track patterns using a simple food journal
How to apply structure without overthinking
-
Use the same breakfast for 3 to 5 days, then adjust if needed
-
Keep lunch and dinner familiar, then rotate one ingredient weekly
-
Maintain one “safe snack” option to avoid random eating
Example
If rice and curd feel stable but raw salad triggers urgency, the fix is not to cut vegetables forever. Cook the vegetables, reduce the portion, and test it with a stable meal.
Once planning becomes consistent, the next layer is learning which dietary supplements can support gut and immune health alongside food.
Beyond Diet Plans: Supplements That May Support Gut and Immune Health
Dietary supplements can help fill nutritional gaps caused by restricted eating or poor absorption. Options like flaxseed oil, chia seeds, and omega 3 fatty acids support inflammation control when used appropriately. Supplements should complement meals rather than replace whole foods.
Supportive nutrition works best when aligned with dietary structure.
When supplements add real value
Supplements help most when symptoms limit food variety, appetite drops, or lab results show deficiencies. Their role is supportive, not corrective.
Common supplements used and their purpose
-
Omega 3 fatty acids support inflammation balance, commonly sourced from fish oil or plant alternatives
-
Flaxseed oil provides a gentle fat source when heavier fats feel difficult to tolerate
-
Chia seeds offer omega fats and fiber, best used soaked and in small portions
How to use supplements without creating new triggers
-
Introduce one supplement at a time
-
Begin with small amounts and adjust gradually
-
Take supplements with meals to reduce stomach irritation
-
Track symptom response for one to two weeks
Example
If fish intake is limited and fat tolerance feels low, flaxseed oil can support intake without changing meals. If chia seeds cause bloating, soaking them and reducing the portion often improves tolerance.
Once supportive nutrition is clear, the next step is shaping a meal plan that adapts smoothly to daily life and symptom changes.
Steps to Personalize a Meal Plan to Manage Ulcerative Colitis Long Term
Personalization turns a general meal plan into a sustainable system. By considering food groups, healthy snacks, lean meats, and individual tolerance, patients can build a meal plan that adapts over time. Long-term success depends on responsiveness rather than rigid rules.
Consistency grows when meals reflect real-world digestion patterns.
1. Identify Personal Trigger Foods
Identifying food triggers requires observation and honesty. Keeping track of reactions helps pinpoint ingredients that consistently cause symptoms.
How to apply this in daily eating
-
Note timing of symptoms after meals
-
Watch for repeat reactions across different days
-
Separate one-time flare sensitivity from consistent triggers
2. Adjust Meals Based on Flare and Remission Phases
During an ulcerative colitis flare, digestion needs rest and simplicity. Meals should shift based on inflammation levels rather than habit.
What usually changes between phases
-
Portion size and texture during flares
-
Variety and nutrient density during remission
3. Balance Macronutrients for Energy and Healing
Proper nutrition ensures energy needs are met without overloading digestion. Balanced macronutrients support tissue repair and immune stability.
What balance looks like
-
Carbohydrates for fuel
-
Protein for repair
-
Fats for sustained energy
4. Prioritize Easily Digestible Foods
Low fiber fruits and soft textures reduce digestive strain. These foods support nourishment while minimizing irritation.
Practical focus
-
Cooked fruits and vegetables
-
Soft grains and mashed foods when sensitivity rises
5. Track Symptoms and Food Responses Consistently
A food journal helps connect symptoms with specific meals. Patterns become clearer when tracked consistently over time.
What to record
-
Food type and portion
-
Preparation method
-
Symptom timing
6. Modify Portion Sizes and Meal Timing
Smaller portions and consistent timing reduce digestive workload. This helps stabilize bowel patterns throughout the day.
Why this matters
-
Large meals stress an inflamed gut
-
Predictable timing supports digestive rhythm
7. Review Nutrient Gaps and Deficiencies
Diet restrictions can create nutrient gaps. Regular review helps prevent long-term deficiencies.
Common signs to watch
-
Fatigue
-
Low appetite
-
Unintended weight change
8. Reintroduce Foods Gradually and Strategically
Other foods can often return slowly once symptoms stabilize. Controlled reintroduction prevents unnecessary restriction.
How to reintroduce safely
-
One food at a time
-
Small portions
-
Several days between tests
9. Align the Meal Plan With Medical Treatment
Meals should support prescribed treatment, not conflict with it. Coordination improves overall disease control.
Simple alignment habits
-
Match meals with medication timing
-
Share diet changes during clinical reviews
10. Reassess and Adapt the Meal Plan Over Time
Digestion changes with disease activity and lifestyle. Reassessment keeps the meal plan effective long term.
What reassessment looks like
-
Monthly reflection on tolerance
-
Adjusting meals during stress or routine shifts
What personalization looks like in practice
Personalization means building repeatable meals first, then widening options with control. The goal is steady digestion, stable energy, and fewer surprise reactions.
How to build your plan without guesswork
-
Keep two to three safe meals that cover core food groups
-
Choose one or two healthy snacks that fit your tolerance window
-
Use lean meats or tolerated proteins to keep meals complete
-
Change one variable at a time, portion, timing, or texture
-
Track reactions until patterns become clear
Example
A person may tolerate rice and soft vegetables at lunch, but react to the same vegetables raw. Cooking and portion control become the personalization tool, not cutting the ingredient forever.
FAQs
1. What Are Some Healthy Foods That Are Generally Well Tolerated During Ulcerative Colitis?
Most people tolerate soft, simply cooked foods such as white rice, oats, cooked vegetables, eggs, fish, tofu, and low fiber fruits. Portion size and preparation often matter more than the food itself.
2. How Long Does It Take to Notice Improvement After Changing Following Foods Consistently?
Early symptom relief often appears within one to two weeks when following foods are adjusted consistently. More stable digestion usually develops over several weeks as inflammation settles.
3. Are Dietary Supplements Necessary if Meals Are Carefully Planned?
Dietary supplements are not always necessary when meals are well planned and tolerated. They become helpful during flares or when digestion limits food variety and absorption.
4. Which Foods Rich in Nutrients Are Often Missed Due to Digestive Restrictions?
Digestive restrictions often reduce intake of fiber rich vegetables, whole grains, omega fat sources, and mineral dense foods. Careful planning helps recover these nutrients without increasing irritation.
5. Can Stress and Eating Speed Affect Symptoms Even With the Right Diet?
Yes. Stress and fast eating increase gut sensitivity and can trigger symptoms even with tolerated foods. Slower, calmer meals often improve digestion without changing the diet.
Conclusion
Eating with ulcerative colitis becomes manageable when decisions are guided by structure rather than fear. A reliable diet plan gives you a starting point, then room to adjust based on how your body responds in real situations.
The most effective next step is simple and practical: choose meals you tolerate, prepare them gently, eat at steady times, and observe patterns instead of reacting to single days.
With consistency, confidence replaces uncertainty, and eating slowly returns to being part of daily life rather than a calculated risk.
Balanced eating is rarely about perfection. It is about patterns that hold. MyBalanceBite is built around that same idea.




















Leave a comment
Translation missing: en.blogs.comments.discription