A single lab report can change how seriously food choices suddenly feel. When cholesterol numbers cross the line, advice needs to move from theory to something that works every day.
This is where a diet plan to reduce cholesterol becomes more than advice. Doctors are recommending plans that work with normal meals, steady routines, and habits people can sustain beyond a few weeks.
What makes this approach stand out is its focus on structure, balance, and long term heart protection. That foundation explains why medical guidance is shifting toward dietary plans built for real life, not temporary control.
What Is Cholesterol?
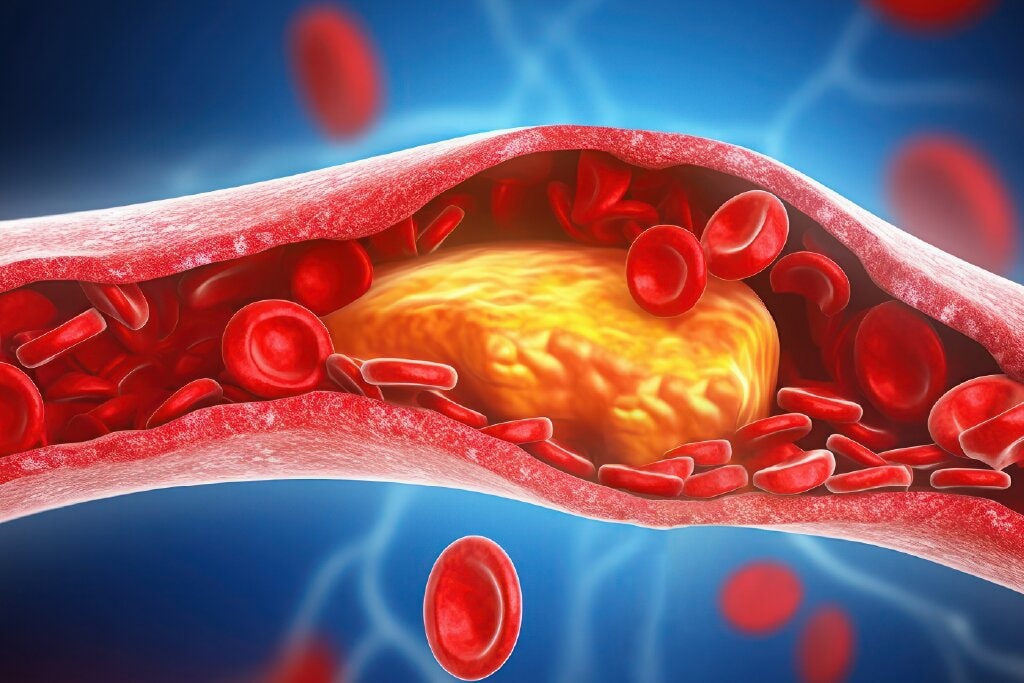
Cholesterol is a waxy substance found in the blood and digestive tract that supports hormone production and cell structure. Problems begin when excess cholesterol builds up, affecting total cholesterol levels and disrupting the healthy range.
Poor cholesterol absorption can lead to plaque formation, especially when low density lipoprotein outweighs high density lipoprotein. Understanding how cholesterol behaves inside the body clarifies where imbalance begins.
What Cholesterol Actually Does
Cholesterol helps the body build cell membranes, produce hormones, and make vitamin D. It also supports bile production, which aids fat digestion. The issue is not cholesterol itself, but how much accumulates and how it circulates inside the bloodstream.
How It Moves Through Your Body
Cholesterol travels through blood using lipoproteins, and the type of carrier determines its effect. For individuals looking to manage cholesterol as part of a weight loss journey, it is important to understand why most diet for obesity fail in the long run and what a clinically proven, sustainable plan does differently.
-
Low density lipoprotein carries cholesterol toward tissues and arteries, which is why it is often called bad cholesterol.
-
High density lipoprotein helps move cholesterol away for processing, which is why it is known as good cholesterol and helps raise HDL cholesterol when supported correctly.
Why Absorption Matters More Than Most People Think
Cholesterol control is shaped heavily by digestion and absorbing cholesterol in the gut.
-
Plant sterols compete during digestion and reduce cholesterol absorption.
-
Soluble fiber binds cholesterol in the digestive tract and helps remove it.
-
Getting more soluble fiber usually comes from foods rich in oats, legumes, and whole grains.
Example
A breakfast of oat bran topped with fresh fruit and a spoon of almond butter adds soluble fiber without feeling restrictive.
A lunch built around kidney beans, whole grains, and citrus fruits supports the same process with variety and balance.
Food Signals That Push Cholesterol in Opposite Directions
Fat quality matters as much as fat quantity.
-
Olive oil and avocado oil support healthier fat balance in meals.
-
Fatty fish provides omega 3 fatty acids that align with long term heart health patterns.
-
Partially hydrogenated oils introduce trans fat, which often raises bad cholesterol.
-
Orange juice and soy milk can fit into meals, but overall food combinations matter more than single items.
Cholesterol becomes easier to manage once you understand the carriers, not just the total number.
That distinction sets the stage for examining how LDL cholesterol and HDL cholesterol affect the body differently.
Build Your Cholesterol-Friendly Plate With MyBalanceBite
LDL Cholesterol vs HDL Cholesterol: Key Differences That Matter
Cholesterol levels are shaped less by totals and more by how cholesterol travels in the body. LDL and HDL play opposite roles, and that difference directly affects heart risk, plaque buildup, and long term cardiovascular balance.
Understanding this contrast helps interpret blood reports with far more accuracy.
| Aspect | LDL Cholesterol | HDL Cholesterol |
|---|---|---|
| Common Name | Bad cholesterol | Good cholesterol |
| Primary Role | Carries cholesterol to tissues and artery walls | Carries cholesterol away for removal |
| Impact on Arteries | Promotes plaque buildup when elevated | Helps clear excess cholesterol |
| Effect on Heart Risk | Higher levels increase risk | Higher levels reduce risk |
| Healthy Range | Below 100 mg/dL is considered optimal | 60 mg/dL or higher is protective |
| Borderline Range | 130–159 mg/dL | 40–59 mg/dL |
| High Risk Level | 160 mg/dL and above | Below 40 mg/dL |
| Desired Direction | Lower is better | Higher is better |
This contrast explains why cholesterol reports cannot be judged by a single number. Once the roles of LDL and HDL are clear, dietary and lifestyle choices start making practical sense. That clarity naturally leads into examining which habits and foods push these markers in opposite directions.
Common Dietary Habits and Lifestyle Factors That Lead to High Cholesterol
High cholesterol develops through a mix of dietary habits and lifestyle risk factors. Regular intake of saturated fat, trans fat, processed foods, unhealthy fats, and foods high in sugar or refined carbs raises excess cholesterol.
Limited physical activity, weight management issues, metabolic syndrome, and daily choices like smoking further accelerate imbalance. Identifying these triggers helps isolate which habits quietly push cholesterol levels upward.
1. Frequent Intake of Saturated and Trans Fats
Saturated fat and trans fat influence how the liver produces and clears cholesterol. When intake is frequent, LDL levels tend to rise regardless of calorie control.
-
Common sources include fried foods, bakery items, and fast food
-
Partially hydrogenated oils remain a major source of trans fat
-
Repetition matters more than portion size on any single day
Example
A daily packaged snack may contribute more trans fat exposure over a week than an occasional restaurant meal.
2. High Consumption of Processed and Packaged Foods
Processed foods often combine refined starch, unhealthy fats, and excess sodium, creating a pattern that steadily disrupts cholesterol balance.
-
Ingredient lists often hide trans fat and saturated fat
-
Low fiber content reduces natural cholesterol clearance
-
Regular intake can also influence blood pressure trends
3. Excessive Sugar and Refined Carbohydrate Intake
High sugar intake affects lipid metabolism by increasing triglycerides and worsening insulin response, which often overlaps with metabolic syndrome.
-
Sugary drinks raise blood sugar quickly and repeatedly
-
Refined carbohydrates reduce satiety and encourage overeating
-
Over time, this pattern strains cholesterol regulation
4. Low Intake of Fiber Rich Foods
Fiber plays a direct role in cholesterol control, particularly soluble fiber, which binds cholesterol during digestion.
-
Soluble fiber supports removal of cholesterol through the gut
-
Low fiber meals increase hunger and snacking frequency
-
Consistent intake improves long term lipid stability
Example
Choosing oats and fruit instead of refined cereal at breakfast can improve fullness and support cholesterol clearance across the day.
5. Sedentary Lifestyle and Lack of Physical Activity
Physical activity supports lipid balance by improving how fats are used and transported in the body. Pairing exercise with a balanced diet plan can further enhance weight management and overall health.
-
Regular movement supports HDL function
-
Post meal activity improves metabolic response
-
Inactivity often pairs with poor sleep and higher stress
6. Excess Body Weight and Abdominal Fat
Abdominal fat influences liver fat processing and increases cholesterol production even when total weight gain is modest.
-
Waist circumference reflects risk more clearly than scale weight
-
Small improvements in weight management affect lipid levels
-
Sustainable habits matter more than rapid loss
7. Chronic Stress and Poor Sleep Patterns
Stress and sleep disruption influence appetite control, food choices, and routine consistency.
-
Poor sleep increases cravings for sugar and refined foods
-
Chronic stress promotes reliance on packaged meals
-
Irregular routines weaken cholesterol control efforts
8. Smoking and Regular Alcohol Consumption
Smoking directly affects blood vessels and HDL efficiency, while excess alcohol raises triglycerides and disrupts fat metabolism.
-
Smoking accelerates cardiovascular risk independently
-
Alcohol adds calories and often displaces balanced meals
-
Both reduce recovery and metabolic resilience
9. Genetic Predisposition and Family History
Some individuals produce more cholesterol naturally due to genetic factors, even with reasonable habits.
-
Early high cholesterol in relatives is a key signal
-
Genetics shape baseline risk, not final outcomes
-
Consistency still improves cholesterol trends
10. Hormonal Changes and Age Related Factors
Hormonal shifts affect fat storage and cholesterol processing, especially with age and metabolic changes.
-
Hormones influence how fats circulate in blood
-
Aging alters cholesterol clearance efficiency
-
Early adjustments reduce long term accumulation
Once these patterns are understood, the focus naturally shifts to what prolonged imbalance does to the body and why cardiovascular risk rises quietly over time.
Long Term Health Risks of Untreated High Cholesterol
Untreated high cholesterol directly increases the risk of heart disease, heart attack, and long term cardiovascular damage. Plaque formation narrows arteries, raising blood pressure and progressing toward high blood pressure over time.
As circulation weakens, the risk of heart complications grows steadily. Recognizing these outcomes explains why cholesterol control is about prevention, not just numbers.
1. Increased Risk of Heart Disease and Heart Attacks
When plaque builds inside arteries, the heart receives less oxygen rich blood, even if daily life feels normal.
-
Arteries lose flexibility, so the heart works harder
-
Blockages reduce blood supply during exertion and stress
-
Risk rises faster when cholesterol stays high for years
Example
Many heart attacks happen in people who felt fine until a blockage crossed a tipping point.
2. Higher Chances of Stroke Due to Blocked Arteries
Cholesterol related plaque can restrict blood flow to the brain or trigger clots that travel upward.
-
Narrowed vessels reduce oxygen delivery to brain tissue
-
Plaque rupture can form clots that block blood supply
-
Stroke risk increases when blood pressure stays elevated
3. Progressive Damage to Blood Vessels and Arteries
High cholesterol changes artery walls gradually, which makes damage harder to notice early.
-
Plaque formation creates chronic irritation inside vessels
-
Inflammation stiffens arteries and affects circulation
-
Vessel damage reduces the body’s ability to regulate flow
4. Worsening Blood Pressure and Reduced Blood Flow
As arteries narrow, pressure rises because the same blood volume must pass through a smaller space.
-
Narrow arteries push blood pressure upward
-
Reduced blood flow affects legs, kidneys, and heart function
-
High blood pressure increases strain on the entire system
5. Greater Risk of Atherosclerosis Over Time
Atherosclerosis is the long process of plaque buildup and artery hardening, and it shapes most serious cholesterol outcomes.
-
Plaque formation becomes more stable and harder to reverse
-
Stiff arteries reduce circulation efficiency
-
Long term buildup increases the risk of heart complications
Once these risks are clear, the next step is choosing a diet approach that lowers cholesterol while protecting heart health through daily food structure.
A Practical Dietary Approach to Lower Cholesterol and Improve Heart Health
A structured diet plan helps lower your cholesterol by focusing on cholesterol lowering foods and a heart healthy eating plan. Heart healthy meals support therapeutic lifestyle changes recommended by the national heart and lung and blood institute under health and human services.
This approach follows the TLC diet framework to promote heart health through consistent food choices.
| Meal Timing | Veg Option: Try this doctor-recommended 7 day diet to lower triglycerides and improve heart health. | Non-Veg Option | Vegan Option |
|---|---|---|---|
| Breakfast | Vegetable oats with skim milk, 1 bowl (40 g oats), ~280 kcal | Vegetable omelette with 2 egg whites, 1 whole egg, 1 slice whole grain toast, ~300 kcal | Oats cooked in soy milk with fresh fruit, 1 bowl, ~290 kcal |
| Mid-Morning | 1 apple or citrus fruit, ~80 kcal | 1 orange or fresh fruit, ~80 kcal | 1 bowl papaya or citrus fruits, ~90 kcal |
| Lunch | Brown rice 1 cup, mixed veg curry, dal ½ cup, ~480 kcal | Grilled fatty fish 100 g, brown rice 1 cup, vegetables, ~520 kcal | Kidney beans curry ¾ cup, brown rice 1 cup, vegetables, ~500 kcal |
| Evening Snack | Roasted chana 30 g, green tea, ~150 kcal | Handful nuts 20 g, green tea, ~180 kcal | Almond butter 1 tbsp on whole grain toast, ~170 kcal |
| Dinner | Whole wheat roti 2, paneer bhurji 100 g, salad, ~450 kcal | Grilled chicken 120 g, sautéed vegetables, 1 roti, ~480 kcal | Stir-fried vegetables with tofu, 2 rotis, ~460 kcal |
| Optional Add-On | 1 tsp olive oil in cooking | 1 tsp olive oil in cooking | 1 tsp avocado oil in cooking |
Want a Personalized Version of This Diet Plan?
MyBalanceBite helps tailor heart-healthy meals based on your lifestyle, preferences, and health goals.
Portion and Nutrient Logic
This plan balances calories across the day while prioritizing soluble fiber, whole grains, and healthy fats. Fatty fish provides omega 3 fatty acids, while beans, oats, and vegetables help reduce cholesterol absorption. Oils are limited to small amounts to support heart health without excess calories.
Example
A vegan lunch with kidney beans and brown rice delivers protein, fiber, and steady energy without relying on saturated fat.
This structure shows how diet choices translate into daily meals, and the next section focuses on foods that disrupt this balance and quietly slow cholesterol progress.
Foods to Avoid That Raise High Cholesterol and Slow Heart Health Progress
Certain foods high in unhealthy fats directly interfere with cholesterol control and heart health. Processed foods, full fat dairy products, coconut oil, salad dressing, and some liquid vegetable oils increase cholesterol levels when eaten frequently.
These choices slow progress even within a balanced diet plan. Knowing what to limit helps protect gains made through healthier eating patterns.
What to Limit First
These are the most common cholesterol disruptors because they raise saturated fat intake, introduce trans fat exposure, or make portion control harder.
-
Processed foods like packaged snacks, instant noodles, and bakery items
-
Full fat dairy products like full cream milk, cheese, butter, and cream based sauces
-
Coconut oil, especially when used daily in high quantity cooking
-
Salad dressing that is creamy, sweetened, or heavily processed
-
Liquid vegetable oils that are repeatedly reheated or used for deep frying
What to Watch on Labels
Ingredient lists often reveal the real issue faster than nutrition claims.
-
Look for partially hydrogenated oils, which signal industrial trans fat
-
Check for repeated use of “hydrogenated” or “shortening” in baked items
-
Spot added sugar and refined starch combinations that keep cravings active
Example
A “healthy” salad can quietly turn heavy when it is topped with creamy salad dressing and paired with fried sides, even if the main meal looks balanced.
Simple Swaps That Protect Heart Health
Smart swaps work because they reduce unhealthy fats without making meals feel restrictive.
-
Replace heavy dressings with lemon, curd, herbs, or light olive oil based mixes
-
Use low fat dairy options more often than full fat dairy products
-
Cook with controlled oil portions instead of relying on deep frying
The moment these foods are reduced, diet structure starts working more predictably.
That is why the next section focuses on the results to expect when a heart healthy diet is followed consistently.
What Results to Expect When You Follow a Heart Healthy Diet Consistently?

A consistent heart healthy diet gradually improves cholesterol levels and helps lower LDL cholesterol without sudden shifts. Blood test results often reflect lower cholesterol over time, alongside measurable health benefits.
While progress varies, steady dietary patterns support lasting change rather than quick swings. Understanding expected outcomes helps align effort with realistic improvements.
1. Lower LDL Cholesterol With More Stable Cholesterol Levels
LDL levels often improve when meals stay consistent and fiber intake rises.
-
Soluble fiber and whole grains support cholesterol clearance
-
Healthy fats help replace saturated fat without extreme restriction
-
Lower cholesterol trends become clearer when food choices repeat daily
Example
A breakfast built around oats, fruit, and nuts often reduces late morning snacking, which supports steadier cholesterol levels.
2. Clearer Blood Test Patterns Over Time
Blood test results begin matching daily habits rather than short term effort.
-
Total cholesterol aligns better with weekly routines
-
LDL movement becomes easier to interpret
-
Testing feels more meaningful when meals stay consistent
3. Better Blood Pressure Support Through Food Structure
Blood pressure often responds when meals shift toward balanced nutrients.
-
Reduced processed foods lower sodium exposure
-
Home cooked meals create steadier intake
-
Improved hydration supports circulation
4. Practical Heart Health Improvements You Can Feel
Heart health gains often appear as better daily energy and stamina.
-
Fewer post meal energy crashes
-
Improved physical activity tolerance
-
More predictable hunger patterns
5. Health Benefits That Reinforce Long Term Consistency
Visible improvements make healthy eating easier to maintain.
-
Reduced cravings as sugar intake stabilizes
-
Smoother digestion with higher fiber intake
-
Faster meal decisions due to clearer structure
Once these results become familiar, the focus naturally shifts to lifestyle choices that help preserve and strengthen these gains over time.
Track Real Progress, Not Just Numbers
MyBalanceBite helps you turn blood test results into clear, actionable food decisions.
Lifestyle Changes That Strengthen a Diet Plan for Lowering Cholesterol
Lifestyle changes amplify the impact of any diet plan by reinforcing daily habits beyond food. Physical activity supports weight management, while therapeutic lifestyle changes stabilize cholesterol responses long term.
Together, these actions improve consistency and reduce reliance on short term fixes.
1. Regular Physical Activity and Daily Movement
Physical activity improves how the body uses fats and supports heart health markers over time.
-
Aim for consistent movement, not occasional intense workouts
-
Include walking, cycling, swimming, or any activity you can repeat
-
Add light movement after meals to support metabolism
Example
A 15 minute walk after lunch is often easier to maintain than weekend only workouts.
2. Maintaining a Healthy Body Weight
Weight management helps the liver regulate fats more efficiently, which supports steadier cholesterol levels.
-
Focus on slow, repeatable changes rather than sudden drops
-
Track waist size if weight changes feel inconsistent
-
Build meals around fiber and protein for longer fullness
3. Managing Stress Levels Consistently
Stress influences cravings, sleep, and routine stability, which affects food choices and consistency.
-
Use one reliable daily stress release habit
-
Keep meal timing steady during busy days
-
Protect evenings from late snacking triggers
4. Improving Sleep Quality and Duration
Sleep quality shapes hunger hormones and decision making, which affects food patterns the next day.
-
Keep sleep and wake times consistent most days
-
Reduce late caffeine and heavy dinners
-
Create a short wind down routine that feels realistic
5. Quitting Smoking and Avoiding Tobacco
Smoking affects blood vessels directly and weakens long term heart protection.
-
Tobacco cessation improves cardiovascular response over time
-
Avoid secondhand exposure when possible
-
Pair quitting support with routine changes to reduce relapse cues
6. Limiting Alcohol Consumption
Alcohol often disrupts sleep, increases late eating, and adds calories without fullness.
-
Limit frequency before focusing on strict quantity
-
Avoid alcohol close to bedtime
-
Choose food before alcohol to reduce impulsive eating
Once these lifestyle habits are in place, your diet plan becomes easier to follow.
FAQs
1. Can Green Tea Support Cholesterol Control Alongside Medical Treatment?
Yes. Green tea can support cholesterol control by helping reduce LDL levels and improving fat metabolism. It works as a supportive habit, not a replacement for medication or a structured diet plan.
2. Are Healthy Fats Safe for People With a History of Heart Conditions?
Yes, when chosen correctly. Healthy fats from sources like olive oil, nuts, seeds, and fatty fish support heart health and can help improve lipid balance when portion sizes are controlled.
3. Is a Low Cholesterol Diet Enough Without Medication in Mild Cases?
In mild cases, a low cholesterol diet combined with lifestyle changes can be sufficient. Regular monitoring is important to ensure cholesterol levels stay within a healthy range over time.
4. How Often Should Cholesterol Levels Be Tested After Dietary Changes?
Cholesterol levels are usually checked after 8 to 12 weeks of consistent dietary changes. This window allows the body enough time to reflect meaningful trends in a blood test.
5. Can Stress and Mental Health Indirectly Influence Cholesterol Levels?
Yes. Chronic stress and poor mental health can disrupt sleep, increase cravings, and weaken routine consistency, all of which indirectly affect cholesterol levels.
Conclusion
The shift in medical advice is rooted in what patients can actually sustain. When a diet plan fits daily routines, supports steady improvement, and reduces the need for constant correction, it earns long term trust.
The most reliable progress comes from following a plan with intention, monitoring results, and adjusting habits with clarity rather than urgency. That steady approach is what turns guidance into lasting heart health.
Looking for Clarity Beyond Generic Diet Advice?
MyBalanceBite focuses on structured nutrition that works long term, not trends that fade.




















Leave a comment
Translation missing: en.blogs.comments.discription